|
4/29/2024 0 Comments Common retrospect for life tidalPSV eliminates the inspiratory hold, making for better synchronisation and automatically adjusting the effective inspiratory time ( T I) as time constants change. 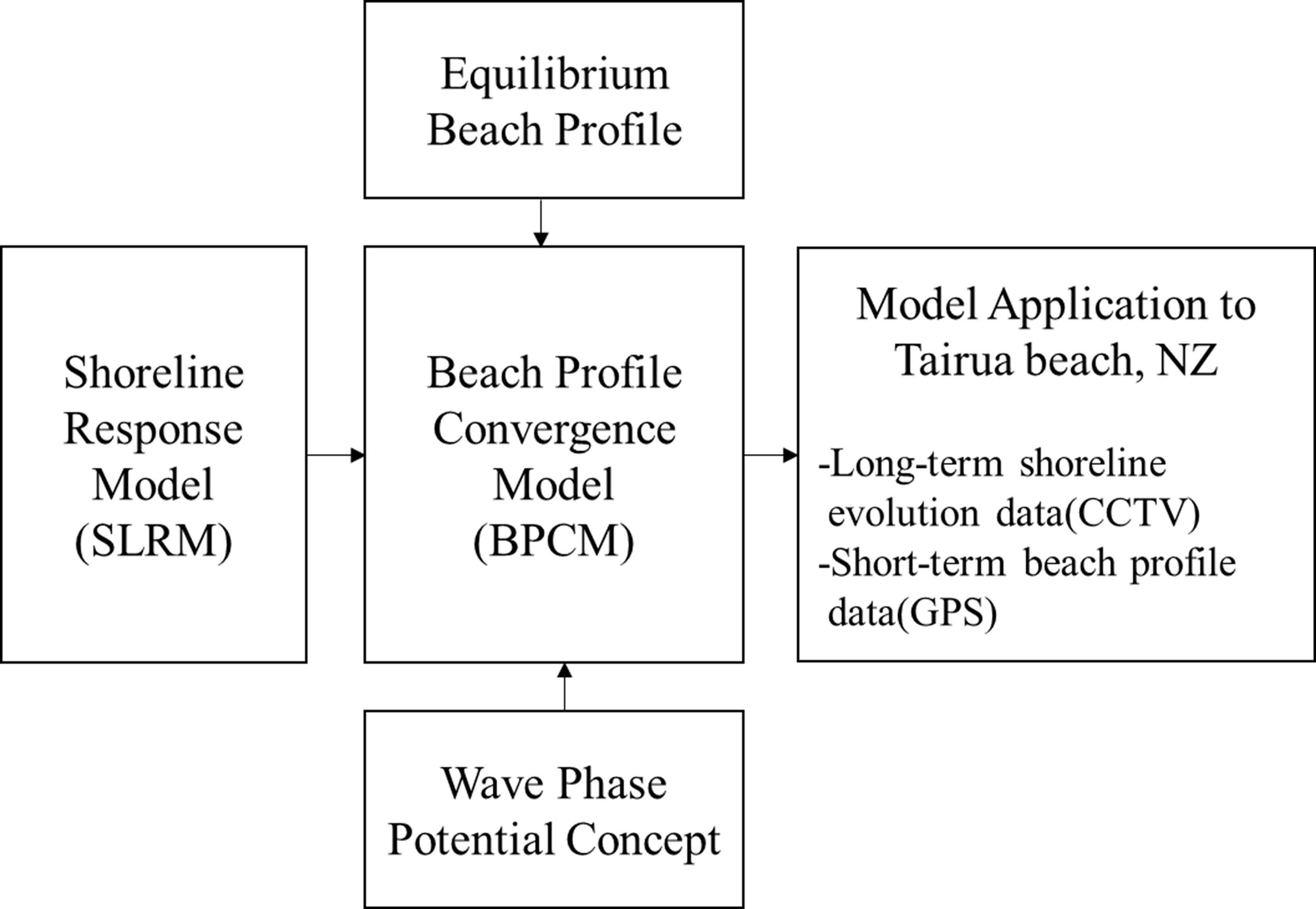
For example, some ventilators make possible the combination of synchronised intermittent mandatory ventilation (SIMV) and pressure support ventilation (PSV), and other ventilators employ PSV as a stand-alone mode with a backup rate, similar to assist/control (AC) but flow rather than time cycled. Although most modern ventilators are capable of providing the basic modes of synchronised (patient-triggered) ventilation, there are a variety of hybrid modes or combinations that may be unique to each manufacturer and device. To a significant degree, the clinician’s choice of ventilator modes is limited by the equipment available in his or her NICU. Settings influenced by whether the obstruction can be relieved by positioning of the endotracheal tube tip beyond the point of maximal narrowing 
Low–medium if obstruction relieved, high otherwise Term infant with oesophageal atresia and tracheomalaciaĪlveolar hypoventilation, expiratory prolongation and gas trapping Low FRC and V T secondary to compromised respiratory muscle functionĪppropriate to give mechanical support for each breathĪlveolar hypoventilation, normal lung compliance Manipulation of pCO 2 can help to control pulmonary blood flow – lower CO 2 to promote blood flow, increase CO 2 to restrict blood flow Lung overdistension with high-pressure settings will restrict pulmonary blood flow. Pulmonary blood flow highly variable and under the influence of intra-alveolar pressure Hypoplastic left heart syndrome, post-Norwood operation Pulmonary atresia with duct-dependent pulmonary circulation Increasing CO 2 can help limit blood flow to some degree Term infant – large ventricular septal defectĭecreased lung compliance related to pulmonary engorgement and oedema Preterm infant – patent ductus arteriosus Reduced pulmonary blood flow secondary to increased pulmonary arteriolar tone V T and PEEP requirements depend on associated parenchymal disease Reduced pulmonary blood flow secondary to increased pulmonary arteriolar tone, exacerbated by low alveolar pO 2 and pH Lungs become relatively compliant once atelectasis resolved, and there is potential for overdistension and volutrauma if pressure settings too high. Global immaturity of respiratory system, with low respiratory muscle capacity High-frequency ventilation (especially HFJV) is preferableĬontinued leak of gas into the pleural spaceĬonsider high-frequency ventilation (if available) where there is a torrential gas leakĮxtremely preterm infant in room air shortly after birth, failing extubation due to inadequate respiratory effort Low PEEP approach may lead to persistent hypoxaemia and respiratory acidosis. Preterm infant with pulmonary interstitial emphysemaĬompression of normal airspaces by interstitial gas Low tidal volumes ( 25 cm H 2O, or if there is refractory hypoxic respiratory failure Limitation of respiratory excursion due to pain Suppression of respiratory drive due to sedation. Lungs often relatively compliant, but potential for overdistension and volutrauma if pressure settings too highĪny infant with a painful surgical incision Should only need low mandatory ventilator rate. Poor respiratory drive, physiological consequences of episodic apnoea (bradycardia and desaturation) 
Preterm infant with apnoea of prematurityĮx-preterm infant with respiratory syncytial virus Predominant pathophysiological disturbance(s)Ĭonsiderations regarding ventilator mode and settings
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
